Vending machines in commercial sex venues to increase HIV self-testing among men who have sex with men
Introduction
Early identification of human immunodeficiency virus (HIV) infection and linkage-to-care is a proven and effective strategy to prevent further transmission of HIV and improve health outcomes. Individuals who are aware of their HIV status are more likely to engage in behaviors that protect their sexual partners such as serosorting or condom use (1). However, barriers prevent people at risk to seek and receive testing services. Those include the availability of services, lack of convenient, private and confidential places (2), and most importantly stigma (3). Novel approaches are necessary overcome those barriers.
Our team used vending machines to distribute home HIV self-test kits to high-risk men who have sex with men (MSM) (4-6). Users characterized the vending machine as an acceptable model of delivering HIV test kits and identified as main advantages the convenience, privacy and confidentiality (5). They also recommended installing the vending machine in places that could ensure privacy. However, limited access to the vending machine and proximity to the target population were important factors that may have influenced the distribution of the test kits. Thus, placing a vending machine strategically in private, non-stigmatizing and easily accessible locations near high-risk populations could assist our efforts in increasing testing for HIV.
Commercial sex venues (CSVs), also known as gay bathhouses and sex clubs, might be an ideal place for such an intervention. Those private establishments have a long history of serving a highly stigmatized and high-risk population (7), as they provide a safe, non-judgmental environment, as well as anonymity and privacy required for sexual intercourse (8,9). A membership or a fee for entrance is necessary to enter the bathhouse. Sex may occur in private rooms, showers, or other public areas, such as orgy rooms or dark mazes. Bathhouses may also offer other services such as swimming pool and Jacuzzis. CSVs are required by Los Angeles County regulations to take preventative measures for HIV and sexually transmitted infections, including signage, free condoms, lubricant and point-of-care testing (10). Alcohol use and illegal drug use are technically not permitted however enforcement is rare. Studies among bathhouse clients reported high-risk sexual behavior, such as sexual encounters with multiple unknown partners, condomless anal sex and drug use (11-13). Additionally, those venues are frequented by a high-proportion of individuals who have not been recently tested for HIV (14).
Our team designed and implemented an intervention that combined home HIV self-test kits with automated vending machines located in two CSVs in Los Angeles, California. The goal of the program was to increase testing uptake among sex club patrons, identify new cases of HIV infection and provide linkage-to-care, when necessary.
Methods
Description of the intervention
The program was conducted between January 2016 and July 2017. Two vending machines (UCapIt, Des Moines, IA, USA) were installed in two CSVs located in downtown Los Angeles. Both machines were located inside the bathhouses in “neutral” areas, such as the on-site STI testing room and the social lounge. The machines were modified to dispense free OrasureTM Oraquick HIV home test kits (Orasure Technologies, Bethlehem, PA, USA). Patrons of the bathhouse visited the vending machine and requested a PIN by sending a text message using their cell phone. Users used the PIN to acquire a test kit free of charge. The withdrawal of multiple tests was allowed and there was no limit to how many times a patron could receive a test kit during the duration of the project.
Each kit contained the manufacturer’s instructions for use and local information about medical assistance in case of a reactive test result. Our team attached also a flyer with an invitation to a secure online survey and stickers with the AIDS Healthcare Foundation (AHF)’s 24/7 Linkage-to-Care hotline.
In the event of a positive or indeterminate/invalid test kit result, participants could ask for further testing in the following ways: (I) use the Orasure contact information; (II) directly contacting the AHF’s 24/7 Linkage-to-Care hotline or (III) provide their contact information during the survey and a program associate would contact them to assist them with further testing and linkage-to-care.
Data collection
All patrons who received a test kit were invited to fill out a 16-item questionnaire using the above-mentioned attached flyer. Survey participants validated their participation by providing their email address, which was used to avoid duplicate participation. The survey included demographic questions (age, gender, race/ethnicity), test kit use and test result. If the reported test result was positive, information about further testing and linkage-to-care was requested. All participants with a reactive result were offered the option for confirmatory testing and linkage-to-care via the AHF. After completing the survey, participants received a $15 electronic gift card. Regardless of their result, at the end of the survey all participants were encouraged to visit AHF’s websites that included information about sexually transmitted infections, HIV and locations of free HIV/STI testing sites.
At the end of the program, baseline survey participants were invited to participate in a second survey. The follow-up questionnaire included questions about test result, current treatment provider if positive, and testing behavior during the past 12 months. A Likert scale was used to record participants’ experience using the vending machine, participating in the program, and testing preferences.
Apart from the surveys, vending machine transactions were recorded remotely via an online platform. This included date and time of dispersal. Multiple test kit requests per participant during the project were permitted.
All databases were extracted to Excel and were analyzed using the IBM SPSS 22.
Costs
We estimated the start-up cost to launch the intervention, which includes the cost of vending machine purchase and installation, and the monthly recurring cost to maintain the project, which included wages, transportation, test kit purchase, and vending machine monitoring service fee. Additionally, we calculated the cost per kit dispensed, by dividing the total cost of the intervention by the number of kits dispensed, the cost per preliminary positive case identified, calculated by dividing cost of the project by the number of self-reported preliminary cases and the cost per case linked by our program, which was calculated by dividing the costs of the program to the number of linked cases.
Program evaluation data
We requested the on-site testing data from the Los Angeles Department of Public Health HIV Testing Services System. Data included all HIV point-of-care testing events, number of positive HIV tests, and demographic information of patrons tested for HIV and patrons with a new positive HIV result between January 1st, 2016 to December 31st, 2016 at the two specific program sites. We requested the same data for all the CSVs in Los Angeles County.
IRB approval
The study was approved by the UCLA Office of Human Research Protection with IRB# 13-000293.
Results
Self-testing uptake and linkage to care
Of the 1,398 test kits dispensed, 110 surveys were completed (response rate: 7.9% of all the patrons who received a kit). Survey participants were men with a median age of 33 years (range, 18–56 years). Most of the participants were Hispanic/Latino (34.5%), followed by White (30%), Black/African Americans (15.5%) and Asian (10%).
The majority of the study participants (91.8%; 101/110) reported that the kit was used and 96 participants (95%; 96/101) reported using the test kit for themselves. Among those who reported using the test kit (101 survey participants), 17 (17.7%) respondents reported a first-time reactive result, two respondents were not sure of the interpretation of their result and in one case the test kit result was reported as invalid.
The preliminary self-reported HIV positive cases were among Latinos (4/17), multiracial (6/17) and white (5/17) men. Among those reporting a reactive HIV result, seven (41%; 7/17) had already sought confirmatory testing or visited a doctor and four of them (24%; 4/17) had initiated treatment for HIV infection. Two survey participants with a reported reactive result were linked to care at AHF utilizing this program. One participant provided his contact info and requested to be contacted by AHF’s Linkage to Care coordinator and the other directly called AHF’s support line.
Participants, who reported they had not used the test kit, were also asked for the reasons not using the test at the time of the study. In total, 14 survey participants reported that they had not used their test kits. In five cases the test kit was used by a friend or partner. Two participants reported that the main reasons for not using the test kit were “I don’t have the time”, “I’m afraid to learn my result”, “I don’t want to learn my result”, but both participants reported they will be using their test kit in the future.
Patterns of vending machine use
During the 18 months of the project, 1,398 kits (nearly 19 kits/week) were dispensed between both CSVs. Kit distribution occurred all days of the week. the days with the highest number of test kit requests were Wednesday (17.7% of distributed kits), Thursday (17.4% of distributed kits) and Saturday (16% of distributed kits). The hours of the day with the highest number of test kit request were 9–10 pm (6.2% of distributed kits) and 3–4 am (5.6% of distributed kits). Nearly 1 out of 5 test kits (21.2%) was requested during hours when point-of-care testing was available.
Follow-up program evaluation survey
All baseline survey participants were invited to participate in a follow-up survey with a flyer attached to the test kit. In total, 12 of 110 men participated (response rate =10.9%). All participants valued their experience using a vending machine to acquire a test-kit and test as “Positive” or “Very Positive”. Using the vending and the self-test kit was easy/very easy (12/13). All would recommend the HIV test kit vending machine to a friend. The attributes that the participants valued most were the convenience of using the vending machine any time they wished, the privacy (“I can test in the location I desire”), quick return of result and control over health decisions. However, respondents were skeptical about the accuracy of their result compared to traditional testing.
Regarding previous testing behavior, 2 out of 12 (16.7%) of the participants had never tested for HIV before this program. Only 3/12 reported that they had ever used the on-site HIV testing services. One person reported that he received his test kit when there was a counselor present. Half of the participants were willing to pay less than $5 (6/12) to obtain a test kit from a vending machine. Finally, 8/12 would prefer self-testing than testing in a clinic.
Cost evaluation
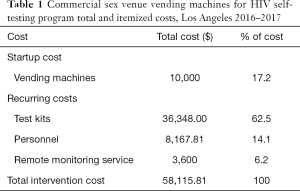
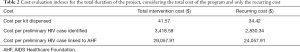
The total cost for the full duration (18 months) of the program was $58,115.81 (Table 1). Each test kit was purchased for $26 and purchasing of the test kits comprised nearly two thirds of the total cost. The cost per kit dispensed when including the total cost of the intervention was $41.57, but when only the recurring cost was included it was $34.42 (Table 2).
Full table

Full table
On site point-of-care testing
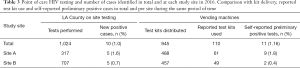
Based on the data extracted from Los Angeles County testing services, 1,024 tests were conducted in these two bathhouses in 2016. Testing identified ten new cases of HIV infection that were linked to medical care (Table 3).
Full table
Discussion
We conducted a pilot project using vending machines to distribute HIV home test kits to patrons of two Los Angeles bathhouses. Our results show that vending machines strategically placed near a high-risk population have the potential to increase HIV testing and identify new cases. Users acquired test kits and the majority of those who self-reported use in survey responses tested near the time of acquisition, while a small number saved them for later use or gave them to their friends. Cases with a preliminary positive result reported that they sought further testing and started treatment. Two participants requested further assistance and linkage through our program. To our knowledge this is the first study presenting the final results of an intervention using vending machines in a CSV. Our team created a novel way to increase testing among a high-risk population alongside currently offered on-site point of care testing. All that, while respecting the privacy and anonymity that patrons seek.
To evaluate the impact of the project in screening for HIV infection and linking to care services, we compared our data to on site point of care testing (Table 3). This involves a rapid test for HIV, along with counseling services. During 2016, the on-site testing at those two CSVs conducted 1,024 tests and identified ten new cases of HIV infection. At the same period, our program dispensed nearly the same amount of self-test kits and identified 11 self-reported preliminary positive cases for HIV infection at a much reduced cost. Our intervention demonstrates the potential to increase testing and identify new cases, in addition to the on-site testing services.
There are only a few reported self-testing interventions in CSVs. Woods et al. (2016) (15) distributed self-test kits in a bathhouse in San Francisco and showed that self-testing has the potential to increase testing and reach high-risk groups and persons that don’t test often. On another study currently in progress in England, Pollard et al. (2018) (16) used vending machines to distribute self-test kits to a gay sauna in United Kingdom. In 6 months of the project, the team dispensed 204 kits, reaching a high-risk population. Uptake was higher via the vending machine compared to the on-site testing at the sauna over the same period (35 vs. 4.56 tests/month). These results show the acceptability, feasibility and effectiveness of testing interventions in similar settings and underline the need for programs located near the high-risk population.
Despite the success in screening, the most important concern was the proper management of cases with an initial positive result. As part of our approach, the pilot program provided information and help for further testing. Despite our efforts to follow up with all the study participants regarding their results, we were unable to verify further testing and linkage to care for most of the cases. We confirmed only two cases that requested assistance from the AHF linkage teams. Loss to follow-up could be addressed by employing smart devices. In a pilot study that included ten participants, Wray et al. (2017) (17) combined a smart-phone application with tracking beacons that notified the team when the self-test kit was opened by the user. Use if this technology enabled the team to perform follow-up and counseling. The intervention was acceptable by the target group and could potentially increase linkage to care.
Another concern was the proper interpretation of the result and the cases of invalid results. The home tests are also designed to be user-friendly and reduce the possibility of misinterpretation (18). As mentioned before, the program provided user-friendly graphical information on testing interpretation along with the already manufacturer-included materials. Additionally, the kit includes easy to understand manufacturer’s instructions on interpretation, as well as a 24/7 phone line, where the user can call for more information. In a previous study, our team showed that MSM who test using a home test kit were willing to provide a photograph of their result using a secure connection from their smartphone (19). A program assistant or an automated algorithm could assist in result interpretation and potentially increase referral to a clinic.
Secondary findings
Costs are important for each public health intervention and strategy design and are always taken into consideration by stakeholders and agencies. The present intervention should be compared to the community programs offering targeted testing services. In a program evaluating HIV point-of care testing in pharmacies and retail clinics (20), the average cost per person tested was estimated at $63.10, after adjusting for inflation (1). That amount included the start-up cost and personnel training. When the recurring costs only were considered (excluding costs for training and reporting), the cost per person tested was $42.94 (2017 US dollars). In another study evaluating the costs of oral fluid testing in community-based clinics (21), the cost per client/patient tested was $36.68 for HIV negative patients and $44.42 for preliminary positive case. Personnel costs accounted for the majority of the testing cost. Our project was characterized by a low startup cost that included mainly the purchase of the vending machines, low maintenance cost, since the vending machines did not require technically complicated training and maintenance by expert staff, and low recurring cost largely dependent on the cost of purchasing test kits.
Our project also provided insights on a population that has not been extensively studied. Studying the patterns of vending machine use, we observed increased test distribution rate may reflect the times when the bathhouses are busy. Interestingly, many kits were acquired late at night and early in the morning. Our concern is that patrons would get a kit at the beginning of night to get tested before having sex to prove to potential partners that they were “infection free”. Perhaps patrons would get another kit before leaving the bathhouse to either test afterwards or test in the future. Unfortunately, we didn’t have the technical capability to monitor when the test kit was used to verify our hypothesis. The UK team that implemented a similar self-testing/vending machine program expressed a similar concern (16). Considering that HIV infection may be missed by the oral fluid test at early stages, the detection capacity of the test, this is an important issue that should be addressed in future interventions with proper education on the importance of frequent testing and protection.
Another observation was that patrons would acquire a test kit, even when point-of-care testing was available on site. Notably, one of the vending machines was located near the point-of-care testing room. Although the number of tests dispensed during testing hours was small, this highlights the importance of offering judgement-free, stigma-free testing that respects anonymity. It should also be noted that test kit distribution was happening 24 hours per day and 7 days a week at times when point-of-care testing was not available (late night hours, holidays, etc.). Self-testing could be an additional strategy to increase the hours testing is offered to a high-risk population, increase locations, offer more privacy.
Our study has certain limitations that should be taken into consideration. First, all survey results are self-reported and the test kit result was self-interpreted, which may result in missed cases. Although test kit instructions were very clear and easy to interpret, our team had no way to verify the positive results of all the preliminary cases. Finally, the small response rate of both surveys does not allow for the generalization of our findings.
While survey response was low, our results demonstrate that an intervention using vending machines and HIV self-test kits in CSVs is acceptable by the high-risk target population and can help identify new HIV cases. We designed a low cost, low maintenance and easy to launch intervention to reach out to populations at-risk for HIV infection, while respecting their privacy. Vending machines could be an opportunity to increase testing for HIV infections or other sexually transmitted diseases among populations or setting with limited availability. Future approaches and programs should focus on ways to increase linkage and retention to care. Programs could benefit from the use of newer technologies, like geotracking devices and smartphones.
Acknowledgements
Funding: This work was supported by the AIDS Healthcare Foundation and UCLA Center for HIV Identification, Prevention and Treatment Services (CHIPTS) (No. P30MH058107).
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The study was approved by the UCLA Office of Human Research Protection with IRB# 13-000293.
References
- Scheim AI, Travers R. Barriers and facilitators to HIV and sexually transmitted infections testing for gay, bisexual, and other transgender men who have sex with men. AIDS Care 2017;29:990-5. [Crossref] [PubMed]
- Bolsewicz K, Vallely A, Debattista J, et al. Factors impacting HIV testing: a review – perspectives from Australia, Canada, and the UK. AIDS Care 2015;27:570-80. [Crossref] [PubMed]
- Levy ME, Wilton L, Phillips G, et al. Understanding structural barriers to accessing HIV testing and prevention services among black men who have sex with men (BMSM) in the United States. AIDS Behav 2014;18:972-96. [Crossref] [PubMed]
- Huang E, Marlin RW, Young SD, et al. Using Grindr, a Smartphone Social-Networking Application, to Increase HIV Self-Testing Among Black and Latino Men Who Have Sex With Men in Los Angeles, 2014. AIDS Educ Prev 2016;28:341-50. [Crossref] [PubMed]
- Young SD, Daniels J, Chiu CJ, et al. Acceptability of using electronic vending machines to deliver oral rapid HIV self-testing kits: a qualitative study. PLoS One 2014;9. [Crossref] [PubMed]
- Young SD, Klausner J, Fynn R, et al. Electronic vending machines for dispensing rapid HIV self-testing kits: A case study. AIDS Care 2014;26:267-9. [Crossref] [PubMed]
- Bérubé A. The History of Gay Bathhouses. J Homosex 2003;44:33-53. [Crossref] [PubMed]
- Haubrich DJ, Myers T, Calzavara L, et al. Gay and bisexual men’s experiences of bathhouse culture and sex: “looking for love in all the wrong places Cult Health Sex 2004;6:19-29. [Crossref] [PubMed]
- Binson D, Woods WJ. A theoretical approach to bathhouse environments. J Homosex 2003;44:23-31. [Crossref] [PubMed]
- County of Los Angeles Department of Public Health Investigation. Part 3 - Bathhouses and Similar Commercial Establishments. Code of Ordinances. Los Angeles County, CA, Municode Library. Available online: https://library.municode.com/ca/los_angeles_county/codes/code_of_ordinances?nodeId=TIT11HESA_DIV1HECO_CH11.04CODICO_PT3BASICOES. Accessed July 5, 2018.
- Grov C. HIV risk and substance use in men who have sex with men surveyed in bathhouses, bars/clubs, and on Craigslist.org: venue of recruitment matters. AIDS Behav 2012;16:807-17. [Crossref] [PubMed]
- Rusow JA, Fletcher JB, Reback CJ. Sexual Venue Choice and Sexual Risk-Taking Among Substance-Using Men Who have Sex with Men. AIDS Behav 2017;21:1149-62. [Crossref] [PubMed]
- Mayer KH, Ducharme R, Zaller N, et al. Unprotected Sex, underestimated risk, undiagnosed HIV and sexually transmitted diseases among men who have sex with men accessing testing services in a New England Bathhouse. J Acquir Immune Defic Syndr 2012;59:194-8. [Crossref] [PubMed]
- Binson D, Woods WJ, Pollack L, et al. Bringing HIV/STI testing programmes to high-risk men. Int J STD AIDS 2005;16:600-4. [Crossref] [PubMed]
- Woods WJ, Lippman SA, Agnew E, et al. Bathhouse distribution of HIV self-testing kits reaches diverse, high-risk population. AIDS Care 2016;28 Suppl 1:111-3. [Crossref] [PubMed]
- Pollard A, Dean G, Soni S, et al. Evaluation of Targeted HIV Self-test Kit Distribution via a Digital Vending Machine. Available online: http://www.croiconference.org/sessions/evaluation-targeted-hiv-self-test-kit-distribution-digital-vending-machine. Published 2018. Accessed July 22, 2018.
- Wray T, Chan PA, Simpanen E, et al. eTEST: Developing a Smart Home HIV Testing Kit that Enables Active, Real-Time Follow-Up and Referral After Testing. JMIR Mhealth Uhealth 2017;5. [Crossref] [PubMed]
- Estem KS, Catania J, Klausner JD. HIV Self-Testing: a Review of Current Implementation and Fidelity. Curr HIV/AIDS Rep 2016;13:107-15. [Crossref] [PubMed]
- Daniels J, Rosengren L, Young S, et al. Will Men Who Have Sex With Men Use Short-Messaging Services to Send Photos of Completed HIV Self-Tests to Researchers? J Assoc Nurses AIDS Care 2016;27:722-6. [Crossref] [PubMed]
- Lecher SL, Shrestha RK, Botts LW, et al. Cost analysis of a novel HIV testing strategy in community pharmacies and retail clinics. J Am Pharm Assoc (2003) 2015;55:488-92. [Crossref] [PubMed]
- Pinkerton SD, Bogart LM, Howerton D, et al. Cost of rapid HIV testing at 45 U.S. hospitals. AIDS Patient Care STDS 2010;24:409-13. [Crossref] [PubMed]
Cite this article as: Stafylis C, Natoli LJ, Murkey JA, Gordon KK, Young SD, McGrath MR, Klausner JD. Vending machines in commercial sex venues to increase HIV self-testing among men who have sex with men. mHealth 2018;4:51.


