
Mobile technology use and mHealth text message preferences: an examination of gender, racial, and ethnic differences among emerging adult college students
Introduction
Mobile health (mHealth) interventions have increased in popularity in recent years to address maladaptive physical and mental health concerns and health behaviors (1,2). In contrast to traditional face-to-face treatment modalities, mHealth interventions enable individuals to receive care in ecologically valid contexts, facilitate hard-to-reach populations’ engagement with healthcare professionals, and can be tailored to meet personal needs and preferences on a momentary basis (3,4). Yet, gaps exist in the literature regarding how to design mHealth interventions in a manner that is apt to be well-received by various targeted populations. Emerging adult college students in general, and minority subgroups in particular, may be especially well-suited to receive mHealth interventions because they commonly experience mental health concerns. In particular, college students report relatively high rates of anxiety (11–17%), depression (14–17%), and suicidality (6–11%) (5,6), and engage in maladaptive health behaviors and inadequate levels of health promoting behaviors (5,7,8), which can adversely impact their psychosocial and physiological well-being. Despite these data, few seek treatment for affective or behavioral concerns (9-11) due to barriers such as stigma, lack of perceived need for care, and time constraints (9). Disconcertingly, male and ethnic minority college students seek and engage in treatment less frequently than female and White students (10,11), highlighting the need for developing novel means of engaging diverse populations in treatment. mHealth platforms can overcome multiple help-seeking barriers (3,4), and thus, may serve as a valuable means of delivering care to these individuals.
Technology use in emerging adults: gender, race, and ethnicity differences
Mobile technologies are ubiquitous in the U.S. and, based on data from 2018, young adults aged 18 to 29 years constitute the highest proportion of adult smartphone owners in the U.S. (12). Young adults aged 18 to 29 years engage with their mobile devices frequently and, in particular, report using such devices for approximately 22.38 hours per week, on average (13). A greater proportion of young adults also engage with various social media platforms on mobile and other web-connected devices than older adults between the ages of 30 and 64 (88% vs. 64–78%) (14). Yet, it remains unclear whether technology use behaviors identified in epidemiological samples of young adults are similar to those of college students. The most recent large-scale data collection on college vs. non-college student technology use patterns provides evidence that college students own and access the internet to a greater degree than age-matched non-students (15), suggesting college students may engage with mobile devices differently than epidemiological samples of general young adults in the U.S.
Gender, racial, and ethnic differences in adults’ technology use have been documented to varying degrees, yet fewer studies have examined these differences among college students. Research suggests gender differences in overall technology adoption among adults have lessened (12,16,17), but variations remain in the ways men and women use mobile devices. For example, male college students more commonly use technology for informational and entertainment purposes, whereas females more often use them for communication and to cultivate relationships (17-20). As advances in technology continuously alter the landscape of the devices and associated applications people adopt, evaluations of students’ engagement with currently available technologies are needed to inform mHealth development.
Racial and ethnic differences in mobile device ownership and time spent online among adults have similarly lessened in recent years (12,16), although this finding may not persist across technology platforms. Data from the Truth Initiative Young Adult Cohort Study conducted in 2016 (n=2,248), for instance, found that non-Latino Black young adults had lower rates of access to internet-enabled smartphones, laptops or desktops, and smart televisions or video game consoles than non-Latino White young adults; Latino young adults similarly exhibited more limited access to internet-enabled laptops or desktops than their White counterparts (21). Although there are no studies of college students conducted within the last decade, a multi-institute assessment of college students collected in 2006–2007 suggests Black students send or receive text messages more often than White students (22). These studies are limited by small samples, decreasing the generalizability and potentially biasing results. Moreover, no studies have yet considered how the use of newer devices (e.g., smartphones) and features [e.g., applications (apps)] differ across racial and ethnic groups in U.S. college students, yet such information can be useful for developing acceptable and effective mHealth treatments for college students.
mHealth interventions for college students
Among college students, empirical studies and systematic reviews suggest that mHealth internet-based and text message-based interventions have been used to decrease alcohol and tobacco use (23-27), reduce eating disorder symptoms (28), improve healthy eating (29), and incite health behavior change (30). Although these studies demonstrate favorable effects for primary and/or secondary outcomes, longer-term health behavior changes remain marginal. Researchers have noted the need to develop new and refine existing interventions, with a particular focus on creating interventions that will be acceptable and usable for college students (23,29,30).
In the first study to evaluate adults’ preferences for text message content in mHealth interventions using quantitative analyses, Muench and colleagues found global preferences for messages that were positive, nonaggressive, grammatically correct, free of textese (texting abbreviations, e.g., LOL), benefit-oriented, polite, and directive (31). These results corroborate the findings from qualitative studies that assessed college students’ text message preferences as part of designing text message-based interventions (32-34), focus group and survey studies among epidemiological and clinical samples of adolescents (35), college students (36-38), and adults (39,40). However, no existing research has used quantitative analyses analogous to Muench and colleagues’ (31) to assess text message preferences among college students, or differences based on participants’ gender, racial, and ethnic identities; such research is needed to inform the development of mHealth interventions for this population.
Study purpose
The present study aimed to examine mobile technology use and text message preferences in a diverse college student sample. Differences in use and preferences were examined by gender (identifying as male or female), race (identifying as Black or White), and ethnicity (identifying as Latino or non-Latino). Based on previous research, we expect most students will own and frequently use smartphones and their features (e.g., text messaging, internet, apps), but rates may vary by gender, racial, and ethnic identities. Specifically, we hypothesize that males will be more likely than females to use smartphones for informational and entertainment purposes, and female students will use these devices for communication and relational purposes to a greater extent than males (17-20). We also expect more White and non-Latino students will own smartphones than their Black and Latino counterparts (21) and, as an exploratory hypothesis, that Black and non-Latino students will be more active smartphone users than White students. Finally, we expect that most students will prefer to receive text messages in the context of mHealth interventions that are positive, short, and lack textese (31) and, in an exploratory fashion, we will examine whether text message preferences vary by gender, race, and ethnicity. This study extends previous work by examining college student technology use differences and preferences among demographic groups, addressing gaps in the literature to better inform the design of mHealth treatments for overlooked college student subgroups in need of care.
Methods
Procedures
Following Institutional Review Board study approval, between July 2015 and April 2016 college students over age 18 from three universities in the Mid-Atlantic U.S. were recruited through flyers, internet advertisements, and a psychology department research pool. As part of a larger study about college student health and experiences, interested students were directed to the Qualtrics online system, where they electronically provided informed consent and completed measures assessing thoughts, feelings, and behaviors related to college student experiences. Participants who completed the survey via the psychology department research pool completed all measures. For those recruited via flyers and internet advertisements, to reduce the survey’s length, we included designed missingness wherein respondents took an abbreviated version of the survey. Specifically, upon beginning the study the Qualtrics software randomized participants to one of two versions of the survey. These two briefer versions were the same length (30 minutes) and were shorter than the survey completed by students in psychology courses (60 minutes). All participants completed the demographics and technology use questionnaires. The text message preference questionnaire was completed by the psychology course participants and half of the general college campus participants. These two recruitment methods (psychology student and general college campus recruitment) were used to increase the sample size and racial diversity.
A total of 2,010 survey responses were initially collected. Participants who provided duplicate entries (n=118), did not provide responses to any questions (n=78), or completed the survey in less than one-third of the median completion time (n=6), were removed. Four validity check items (e.g., “select 2 for this item”) were included in the survey; participants who responded incorrectly to more than one validity item (n=76) and those who did not respond correctly to one of the first two validity items (n=87) were also removed. Finally, to focus on the experiences of emerging adults, respondents over age 25 were excluded (n=274). The remaining 1,371 responses were included in the analyses. As expected, using multiple recruitment methods increased sample size and racial diversity; in the general college campus sample, a greater proportion of participants were Black than White (Black=54.41%, White=45.59%) compared to the proportion of Black students in the psychology student sample (Black=40.28%, White=59.72%; χ2=24.00, P<0.001).
Participants
Participants included 1,371 college students ages 18–25 (20.54±1.80) years. Participants were asked to identify their gender; 24.58% identified as male (n=337), 74.91% identified as female (n=1,027), and 0.51% indicated they preferred not to answer (n=7). Respondents were able to select as many racial identities as applied to them; a similar number of students identified as White/Caucasian (n=679; 49.53%) or Black/African American (n=602; 43.91%), with the remainder reporting Asian/Asian American (n=85; 6.20%), other race (n=79; 5.76%), American Indian/Alaskan Native (n=46; 3.36%), and Native Hawaiian/Pacific Islander (n=12; 0.88%) identities. Regarding ethnic identity, 109 (7.95%) identified as Hispanic/Latino and 1,262 (92.05%) as non-Hispanic/Latino. Most respondents were full-time students (n=1,305; 95.19%) and identified as heterosexual (n=1,050; 76.59%). Similar numbers of students were completing their freshman (n=431; 31.44%), sophomore (n=311; 22.68%), junior (n=330; 24.07%), and senior (n=281; 20.50%) years of undergraduate education.
Measures
Technology use
To augment the current understanding of college students’ technology use, participants were asked to report on their mobile device ownership and technology-related behaviors. Regarding the former, the type of mobile phone(s) participants possessed (general, smartphone), the smartphone type (if applicable, Apple, Android, Windows, Blackberry, Other), the nature of their contracts (long-term, pay-as-you-go), and aspects of their coverage plans (unlimited features, frequency of phone number changes) were assessed. Likewise, the frequency with which respondents use cell phones was assessed, as was how often they send or receive text messages, access email, use the internet, and use apps on mobile devices. Response options fell on a 5-point response scale for cell phone use frequency (response options: I never/rarely use, A few times a month, A few times a week, About once a day, More than once a day) and a 6-point response scale for the remaining frequency variables (response options for each question: I never or rarely use, A few times a year, A few times a month, A few times a week, About once a day, More than once a day). Further, among respondents who endorsed using apps on their mobile devices, the type(s) of app(s) that individuals use were assessed. Specifically, the following app types were assessed: productivity (calendar, alarms, list-making); social media (Facebook, Instagram, Twitter); health and lifestyle (diet, weight, physical activity, and/or sleep tracking); dating (Tinder, OkCupid, Match); entertainment (games, music, watching sports); video recording (YouTube, Vine, Game Your Video); travel or weather (maps, traffic-checking, weather); news (news reports); food and dining (finding restaurants, recipes); finance (banking apps); shopping (Amazon, eBay, Zappos, Etsy).
Message preferences
Eight corresponding text message pairs were adopted from Muench and colleagues (31). The messages in each pair differed on the basis of a specific element related to content or linguistic characteristics. The instructions for these questions read: “Sometimes, as part of a research study the researchers may contact you via text messaging or email. This contact may just be to arrange appointments, but the researchers may also send you messages as part of the study, for example, as a way to help you change your habits or behaviors. The following questions are designed to help us understand your preferences for message styles. For each pair of messages below, please select which one you would prefer to receive from the staff of a research project.” Respondents then indicated which message in each pair they would rather receive. Message content was derived from behavior change and motivational theories, and linguistic variations stemmed from prior research on message preferences and public health messaging campaigns (31).
Data analytic plan
A dichotomous variable was created for gender (self-identify as male n=337, female n=1,027). Responses for individuals who preferred not to answer this question (n=7) were not included in the gender difference analyses but were in all other analyses. Next, although participants could select multiple racial categories, more than 90% identified as Black and/or White. Our analyses of race differences were thus restricted to these two racial groups and, further, were limited to participants who exclusively selected Black (n=563) or White (n=640) to eliminate overlap and were coded in a new dichotomous variable reflecting exclusively Black, or exclusively White. Similar to our approach with gender, 43 respondents who endorsed both Black and White races and 125 participants who endorsed non-Black or non-White racial groups were not included in the race difference analyses. In line with the U.S. Census Bureau’s distinction between race and ethnicity (41), we examined ethnic group differences independent from race for Latino (n=109) and non-Latino (n=1,262) participants. No missing data were present for this ethnicity variable.
A series of chi-square tests of independence were run to examine whether male/female, Black/White, and Latino/non-Latino differences existed for our outcome variables (mobile phone and plan characteristics, technology use frequencies, app types used, and text message preferences). Preliminary inspection of the data revealed heavy skew for the frequency variables, with the vast majority (>90%) reporting use of their cell phones, for example, on an at least daily basis. Response options for all frequency variables (frequency of cell phone use, and texting, email access, internet and app use via mobile devices) were therefore dichotomized to less than daily vs. daily or more. Further, the data used in the current study stem from a larger assessment battery of college student experiences. As described above, the survey included designed missingness to reduce length; all participants completed the demographic and technology measures, but not all completed the text message preference questions. Only participants who completed the text message preference questions were included in relevant analyses (n=1,059; 77.24%). Otherwise, the amount of missing data was negligible (≤0.34% across all variables) and omitted via listwise deletion. Unless indicated, all assumptions for the analyses were met. Given the large number of planned analyses, to reduce our type I error rate, we selected a more stringent alpha level of 0.01 when interpreting significant results. We chose this approach over a more conservative Bonferroni correction given the exploratory nature of the analyses, so as not to miss any potentially meaningful and clinically relevant effects.
Results
Mobile phone and plan characteristics
Table 1 presents overall trends and gender, racial, and ethnic differences in students’ mobile phone and plan characteristics, frequencies of mobile technology use, and use of specific app types. Certain between-group analyses could not be calculated due to small sample sizes (e.g., non-smartphone owners) and when the assumption that all cells in a 2×2 table need an expected frequency ≥5 was not met (42). Overall, 99.5% of students reported owning a smartphone, and among these, 75.9% owned Apple-brand smartphones and 23.3% owned Android-brand smartphones. Chi-square tests are presented in Table 1, comparing phone ownership between genders, races, and ethnicities. Most participants (89.5%) had long-term mobile phone contracts. As the ability to maintain contact with participants in mHealth studies is critical, participants who endorsed having pay-as-you-go plans (n=136) were asked whether their mobile phone numbers change, on average, at least once per year or less frequently; 12.5% reported their mobile phone number changed at least once per year. Among participants with long-term contracts (n=1,165), 94.6% had unlimited texting in their mobile phone plans and 38.6% had unlimited data; there were several significant gender and race group differences in mobile phone plan characteristics, which are presented in Table 1.
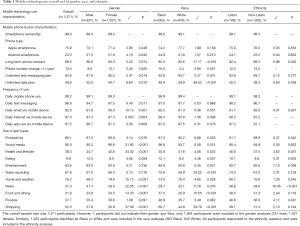
Full table
Mobile technology use
As shown in Table 1, overall 99.2% of students reported using their mobile phones at least once per day and, in particular, 96.8% reported that they send or receive text messages on their mobile devices daily. Most students (92.0%) also reported accessing email on their mobile devices at least once per day. When asked how often they use the internet on mobile devices, 97.3% of participants indicated that they do so daily or more often, and most (97.2%) also reported using apps on mobile devices at least once per day. Comparisons of students’ texting, email and internet access, and app use frequencies by gender, racial, and ethnic groups are reported in Table 1.
The types of apps participants reported using on mobile devices were also examined (n=1,371). Of all apps considered, the highest proportion of students used social media apps (95.0%), followed by productivity (90.1%), entertainment (83.6%), travel and weather (76.2%), video recording (67.8%), and shopping (52.0%) apps. Fewer students endorsed use of health and lifestyle (38.3%), finance (37.7%), food and dining (31.8%), news (31.3%), and dating (9.9%) apps. Rates of use of each app type by students’ gender, racial, and ethnic identities are reported in Table 1.
Text message preference
Table 2 presents overall trends and gender, racial, and ethnic differences in students’ preferences for which text messages in eight mirrored pairs they would rather receive during a hypothetical mHealth intervention. First, stylistic and structural differences in text message preferences were examined. Most (98.9%) preferred a non-textese vs. a textese message. In another dyad, similar numbers of students preferred long (52.1%) and short (47.9%) messages. Preferences based on message emphasis and valence were subsequently examined. In a pairing containing messages with a single vs. multiple exclamation marks, 60.1% of students preferred the former, and most participants (73.8%) also preferred a message containing a smiley face emoticon over a message without an emoticon. In another dyad, more participants preferred a message with capitalization for emphatic purposes (55.0%) over a message without capitalization (45.0%). Message preferences based on tone were evaluated next. First, 75.8% of students preferred a message containing a statement vs. a question and 69.2% of participants preferred a polite message over a message containing the same general request without “please”. Also, 70.0% of students preferred a non-directive vs. a directive message. Gender, racial, and ethnic differences in preferences for each text message pairing are reported in Table 2.
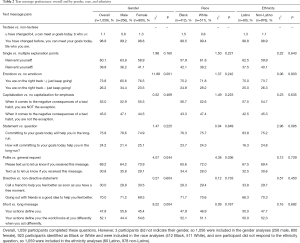
Full table
Discussion
mHealth interventions are a potentially feasible way of targeting emerging adult college students’ physical and mental health concerns, decreasing health-risk, and augmenting health promoting behaviors (2,30). To further the field’s understanding of how to design mHealth treatments in a manner apt to be well-received by college students, the current study expands existing research by examining gender, racial, and ethnic differences in emerging adult college students’ mobile device ownership and usage patterns. The present study also expands the work of Muench and colleagues (31) by considering text message preferences in a large, racially and ethnically diverse sample. Results suggest students frequently use smartphones and inherent features, and that smartphone ownership and plan attributes, usage patterns, and text message preferences vary based on students’ gender, racial, and ethnic identities.
Overall mobile phone, plan, and use characteristics
Not surprisingly, most participants owned smartphones, had long-term mobile phone contracts, and had unlimited text message plans, which attests to the ubiquity of mobile technology in students’ lives. Nearly all students (99.5%) owned smartphones, which exceeds rates reported in epidemiological studies of young adults (87–94%) (12,21). This suggests smartphones are more commonly owned by college students than age-matched non-students and may serve as an advantageous outlet for delivering interventions to college students in particular. Considered alongside the low help-seeking rates for in-person treatment among college students (9-11), and that use of mobile technology can overcome common barriers to seeking in-person care, such as personal stigma and time constraints (3,4), employing mHealth treatments to augment this population’s health may be worthwhile.
Mobile technology ownership, plans, and use rates by gender, race, and ethnicity
Although there were no gender, race, or ethnic differences in mobile phone ownership, this study found gender and race differences in mobile phone plan attributes and usage patterns. First, consistent with the few studies on this topic (17-20), more female than male participants were “mediated communicators” (19) who more frequently used mobile devices for communication (daily texting and emailing), had higher rates of unlimited text and data plans, and more commonly used social media apps, with the daily texting, and unlimited text and data plan differences trending toward significance (P<0.05). With the exception of having unlimited data, however, most female and male participants frequently used these features (>87%). Future research examining the value of adding social connectivity features in mHealth treatments targeting females vs. males can help determine whether they are better received by females or whether such programs may be favorably received across genders.
Racial and ethnic differences in technology use have also been inadequately assessed to date. The current study expanded this very limited literature by finding more Black than White participants used the internet on mobile devices daily, and there were no racial or ethnic differences in daily texting, email, and app use, or ethnic differences in internet use. Furthermore, more Black than White students had unlimited data plans. Our former findings contrast what is, to our knowledge, the only extant study on this topic, wherein Black college students reported texting more often than White students (22). This prior study conducted in 2006–2007 did not assess students’ mobile device-based email, internet, or app use, though, and included small samples Black and Latino students, which may have biased their results. The lack of research in this area necessitates future work to replicate our findings and examine whether similar technology use behaviors, overall, exist among racial and ethnic groups as these findings suggest.
The apps participants reported using in this research lend insight into features that, if used in mHealth development, may increase treatment acceptability. Nearly 40% of participants reported using Health and Lifestyle apps, suggesting a sizable proportion of college students may value improving their health by using apps. Further, more female than male students used these apps and there was a trend for more White than Black students to report such use. These data provide initial evidence suggesting that some subgroups of college students may be more or less inclined to use health-related apps. Such information can be useful if researchers are targeting specific groups of college students for health behavior change interventions (e.g., women, men, racial minorities), as it indicates that some (e.g., women) may be more willing to use health-related apps whereas others (e.g., men) may be less inclined and thus, potentially more difficult to engage in mHealth treatments that use apps or similar technological approaches.
Text message preference by gender, race, and ethnicity
As mHealth interventions often incorporate text messages (1,2), identifying preferences for text message types are indicated. In the current study, most participants preferred messages with statements, a smiley face emoticon, a single exclamation mark, capitalization, and those that were non-directive, polite, long, and lacked textese. With few exceptions, these results align with the only extant study that assessed text message preferences via quantitative analyses (31), and research that evaluated text message preferences through focus groups and other qualitative methods (32-35). Participants’ preferences for messages that were longer, non-directive, and had a smiley emoticon, however, contrasts some prior studies that primarily employed small focus groups of college students (32,33). The present study found more females than males preferred the longer message, which contrasts two prior studies of college students using majority female focus groups and exhibited preferences for brief and concise messages (32,33). Preferred text message length, then, may be idiosyncratic, rather than generalizable at the population or group level.
Differences in preferences for non-directive and directive messages between the current and prior studies may stem from differing definitions of “directive” and the samples used. Although previous research suggested directive messages were preferred by adults (particularly older adults), these individuals were more averse to commands for immediate action (31). Students’ preference for the non-directive message is interesting to consider alongside their concomitant endorsement of the declarative statement over a reflective question. These data paradoxically suggest that college students may want to avoid spending time contemplating steps they can take to make health changes and are open to informative statements about behavior change, yet do not wish to explicitly be told what to do. Researchers and clinicians who implement mHealth programs should be aware that if behavioral treatments are disseminated via text message, students may be more receptive if the language is tempered so that information and suggestions are offered, and less open to either reflective questions or commands.
Most respondents in the present study preferred a message with a smiley emoticon over no emoticons, and more females than males exhibited this preference. These results add to a small and equivocal literature in this area (32,35). Perhaps the general proclivity towards positive messages seen in the message preference literature more broadly accounts for the present findings (31,33,35), as smiley emoticons are positive in nature. This latter assertion is corroborated by our result that students preferred a polite message over a request without the word “please”. Our results, then, likely reflect students’ preference for positive messages, and using a positive tone in mHealth text message programs for college students may prove beneficial.
Clinical and research implications
The present study may inform the design and implementation of mHealth interventions on college campuses, as it demonstrated that racially diverse emerging adult college students have high smartphone ownership and usage rates, and unique preferences for text messages that may be implemented in new or via refinements to existing mHealth interventions. The pervasiveness of such ownership and use identified in the present study, for one, is particularly noteworthy in light of evidence that adults with racial and ethnic minority identities exhibit poorer physical and mental health and engage with healthcare services less frequently than their majority counterparts (10,11,43). As such, employing mobile technology to deliver health-related interventions to these populations may prove particularly advantageous in advancing the holistic health of minority groups in need of care. Of note, ecological momentary interventions (EMI), just-in-time interventions (JIT), and just-in-time adaptive interventions (JITAI) are increasingly used to prevent and treat physical and mental health concerns and for health behavior change (3,44). These interventions use mobile devices to actively (e.g., self-report) and/or passively (e.g., GPS, accelerometers) assess, and adapt treatments to, individuals’ psychophysiological states and sociocultural contexts (44). When developing EMI, JIT, or JITAI for emerging adult college students, researchers may benefit from the present results that suggest certain student groups have and use various technology features more often than others, and subsequently incorporate these elements to enhance treatment acceptability. It may be particularly useful to determine whether including aspects of the app types commonly used by college students (and specific gender, racial, and ethnic groups) increases treatment engagement. For example, in the present study the most commonly used app types by students overall (>83%) were social media, productivity, and entertainment apps, and as prior research suggests college students frequently use social networking sites and instrumental and recreational features on their mobile devices (17), it may be beneficial to test whether incorporating “fun” app features (social networking, music, games) within mHealth interventions increases their acceptability among college students. In support, recent evidence suggests that mHealth and eHealth interventions that incorporate apps with social networking (e.g., peer chat, team challenges) and gamification (e.g., “exergames”) features is associated with improvements in dietary, physical activity, and sedentary behaviors in the short-term (45,46). Determining how to aptly sustain such health behavior changes in the long-term, perhaps through the use of booster sessions that incorporate these “fun” app features, is a vital feat for the field moving forward. Finally, the present study also found a relatively higher proportions of female, Black, and Latino students used social media and/or entertainment apps than male, White, and non-Latino students. It could thereby prove beneficial to further assess whether including “fun” app features is more useful among the former groups, and to examine the impact on treatment engagement and both short- and long-term physical and mental health outcomes.
Limitations and future directions
This exploratory study adds to the underdeveloped literature on gender, racial, and ethnic differences in emerging adult college students’ mobile device ownership and plan attributes, usage patterns, and text message preferences, and should be confirmed and extended in future research. Our analyses were limited to female and male, White and Black, and Latino and non-Latino groups, and included few Latino students, which may have biased our results or limited generalizability. This was a non-random volunteer sample and we had more female than male participants. Future research should discern if our results differ among other minority groups to inform mHealth development for a broader array of students needing care. This study was also descriptive and cross-sectional, such that our results cannot be linked to mHealth treatment outcomes; longitudinal research can establish causal relations between our descriptive findings and mHealth treatment outcomes. Participants’ text message preferences were also not evaluated in vivo during a mHealth intervention but provided information about general preferences for text message types that may be relevant to include in future mHealth interventions. Whether attending to these stylistic preferences impacts mHealth treatment outcomes among students should be explored in future research. Finally, future research examining other aspects of feasibility and acceptability of mHealth interventions for diverse college student groups is needed. For example, considering students’ perceived need for and readiness to change, willingness to use mHealth interventions, optimal devices and formats for delivering interventions, and barriers of use are all key factors that should be assessed in future work.
Conclusions
This study provides evidence that smartphones are commonly used by college students and may be a feasible platform for health intervention delivery among diverse students. The present findings suggest college students have high rates of smartphone ownership, text frequently, have unlimited text plans, and have long-term phone contracts. mHealth interventions delivered via apps could capitalize on the present results by assessing whether incorporating aspects of the app types commonly used by students overall, and potentially tailoring for specific gender, racial, and ethnic groups, increases mHealth engagement and intervention efficacy. Finally, the text message preference results support use of proper syntax and a positive tone when designing mHealth text message interventions for college students. Collectively, this research can be used to increase the acceptability, usability, and efficacy of mHealth treatments for college students in both general and minority student groups.
Acknowledgements
This work was supported by a grant from the Old Dominion University Office of Research to KE Heron.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: This study was approved by the Institutional Review Boards of Old Dominion University (IRB approval #754356), Norfolk State University (IRB approval #15-08) and Virginia Wesleyan University. Informed consent was obtained from all participants before enrollment into the study.
References
- Fiordelli M, Diviani N, Schulz PJ. Mapping mHealth research: A decade of evolution. J Med Internet Res 2013;15:e95. [Crossref] [PubMed]
- Hall AK, Cole-Lewis H, Bernhardt JM. Mobile text messaging for health: A systematic review of reviews. Annu Rev Public Health 2015;36:393-415. [Crossref] [PubMed]
- Heron KE, Smyth JM. Ecological momentary interventions: Incorporating mobile technology into psychosocial and health behaviour treatments. Br J Health Psychol 2010;15:1-39. [Crossref] [PubMed]
- Price M, Yuen EK, Goetter EM, et al. mHealth: A mechanism to deliver more accessible, more effective mental health care. Clin Psychol Psychother 2014;21:427-36. [Crossref] [PubMed]
- American College Health Association (ACHA). ACHA-National College Health Assessment II: Reference Group Executive Summary Spring 2016. Hanover, MD: ACHA; 2016.
- Eisenberg D, Hunt J, Speer N. Mental health in American colleges and universities: Variation across student subgroups and across campuses. J Nerv Ment Dis 2013;201:60-7. [Crossref] [PubMed]
- Kritsotakis G, Psarrou M, Vassilaki M, et al. Gender differences in the prevalence and clustering of multiple health risk behaviours in young adults. J Adv Nurs 2016;72:2098-113. [Crossref] [PubMed]
- Kang J, Ciecierski CC, Malin EL, et al. A latent class analysis of cancer risk behaviors among US college students. Prev Med 2014;64:121-5. [Crossref] [PubMed]
- Eisenberg D, Hunt J, Speer N. Help seeking for mental health on college campuses: Review of evidence and next steps for research and practice. Harv Rev Psychiatry 2012;20:222-32. [Crossref] [PubMed]
- Lipson SK, Kern A, Eisenberg D, Breland-Noble AM. Mental health disparities among college students of color. J Adolesc Health 2018;63:348-56. [Crossref] [PubMed]
- Hunt JB, Eisenberg D, Lu L, et al. Racial/ethnic disparities in mental health care utilization among US college students: Applying the Institution of Medicine definition of health care disparities. Acad Psychiatry 2015;39:520-6. [Crossref] [PubMed]
- Pew Research Center. Mobile fact sheet. 2018 [cited 2018 December 26]. Available online: https://www.pewinternet.org/fact-sheet/mobile
- Lopez-Fernandez O, Kuss DJ, Romo L, et al. Self-reported dependence on mobile phones in young adults: A European cross-cultural empirical survey. J Behav Addict 2017;6:168-77. [Crossref] [PubMed]
- Smith A, Anderson M. Social media use in 2018. Pew Research Center; 2018 [cited 2019 January 4]. Available online: http://www.pewinternet.org/2018/03/01/social-media-use-in-2018/
- Smith A, Rainie L, Zickuhr K. College students and technology. Pew Research Center; 2011 [cited 2018 September 23]. Available online: https://www.pewinternet.org/2011/07/19/college-students-and-technology/
- Anderson M. Demographics of device ownership. Pew Research Center; 2015. [cited 2018 September 23]. Available online: http://www.pewinternet.org/2015/10/29/the-demographics-of-device-ownership/
- Joiner R, Stewart C, Beaney C. Gender digital divide: Does it exist and what are the explanations? In: Rosen LD, Cheever N, Carrier ML, editors. The Wiley Handbook of Psychology, Technology and Society. Malden, MA: Wiley; 2015;74-88.
- Grellhesl M, Punyanunt-Carter NM. Using the uses and gratifications theory to understand gratifications sought through text messaging practices of male and female undergraduate students. Comput Human Behav 2012;28:2175-81. [Crossref]
- Kimbrough AM, Guadagno RE, Muscanell NL, et al. Gender differences in mediated communication. Comput Human Behav 2013;29:896-900. [Crossref]
- Linnhoff S, Smith KT. An examination of mobile app usage and the user’s life satisfaction. J Strategic Mark 2017;25:581-617. [Crossref]
- Villanti AC, Johnson AL, Ilakkuvan V, et al. Social media use and access to digital technology in US young adults in 2016. J Med Internet Res 2017;19:e196. [Crossref] [PubMed]
- Junco R, Merson D, Salter DW. The effect of gender, ethnicity, and income on college students' use of communication technologies. Cyberpsychol Behav Soc Netw 2010;13:619-27. [Crossref] [PubMed]
- Berman AH, Gajecki M, Sinadinovic K, et al. Mobile interventions targeting risky drinking among university students: A review. Curr Addict Rep 2016;3:166-74. [Crossref] [PubMed]
- Riley W, Obermayer J, Jean-Mary J. Internet and mobile phone text messaging intervention for college smokers. J Am Coll Health 2008;57:245-8. [Crossref] [PubMed]
- Bock BC, Barnet NP, Thind H, et al. A text message intervention for alcohol risk reduction among community college students: TMAP. Addict Behav 2016;63:107-13. [Crossref] [PubMed]
- Cadigan JM, Martens MP, Dworkin E, et al. The efficacy of an event-specific, text message, personalized drinking feedback intervention. Prev Sci 2018. [Epub ahead of print]. [Crossref] [PubMed]
- Bernstein MH, Stein LAR, Neighbors C, et al. A text message intervention to reduce 21st birthday alcohol consumption: Evaluation of a two-group randomized controlled trial. Psychol Addict Behav 2018;32:149-61. [Crossref] [PubMed]
- Saekow J, Jones M, Gibbs E, et al. StudentBodies-eating disorders: A randomized controlled trial of a coached online intervention for subclinical eating disorders. Internet Interv 2015;2:419-28. [Crossref]
- O'Brien LM, Palfai TP. Efficacy of a brief web-based intervention with and without SMS to enhance healthy eating behaviors among university students. Eat Behav 2016;23:104-9. [Crossref] [PubMed]
- Johnson KF, Kalkbrenner MT. The utilization of technological innovations to support college student mental health: Mobile health communication. J Tech Hum Serv 2017;35:314-39. [Crossref]
- Muench F, van Stolk-Cooke K, Morgenstern J, et al. Understanding messaging preferences to inform development of mobile goal-directed behavioral interventions. J Med Internet Res 2014;16:e14. [Crossref] [PubMed]
- Reese JM, Joseph RP, Cherrington A, et al. Development of participant-informed text messages to promote physical activity among African American women attending college: A qualitative mixed-methods inquiry. J Transcult Nurs 2017;28:236-42. [Crossref] [PubMed]
- Thomas K, Linderoth C, Bendtsen M, et al. Text message-based intervention targeting alcohol consumption among university students: Findings from a formative development study. JMIR Mhealth Uhealth 2016;4:e119. [Crossref] [PubMed]
- Wright CJ, Dietze PM, Lim MS. Beyond basic feedback in mobile brief interventions: Designing SMS message content for delivery to young adults during risky drinking events. JMIR Mhealth Uhealth 2017;5:e79. [Crossref] [PubMed]
- Woolford SJ, Barr KL, Derry HA, et al. OMG do not say LOL: Obese adolescents' perspectives on the content of text messages to enhance weight loss efforts. Obesity 2011;19:2382-7. [Crossref] [PubMed]
- Bock BC, Rosen RK, Barnett NP, et al. Translating behavioral interventions onto mHealth platforms: Developing text message interventions for smoking and alcohol. JMIR mHealth uHealth 2015;3:e22. [Crossref] [PubMed]
- Kazemi DM, Borsari B, Levine MJ, et al. Real-time demonstration of a mHealth app designed to reduce college students hazardous drinking. Psychol Serv 2018. [Epub ahead of print]. [Crossref] [PubMed]
- Yan AF, Stevens P, Wang Y, et al. mHealth text messaging for physical activity promotion in college students: A formative participatory approach. Am J Health Behav 2015;39:395-408. [Crossref] [PubMed]
- Ahlers-Schmidt CR, Hart T, Chesser A, et al. Content of text messaging immunization reminders: What low-income parents want to know. Patient Educ Couns 2011;85:119-21. [Crossref] [PubMed]
- Ramirez M, Wu S, Beale E. Designing a text messaging intervention to improve physical activity behavior among low-income Latino patients with diabetes: A discrete-choice experiment, Los Angeles, 2014–2015. Prev Chronic Dis 2016;13:E171. [Crossref] [PubMed]
- US Census Bureau. Race and ethnicity. US Census Bureau; 2012 [cited 2018 September 23]. Accessed from: https://www.census.gov/mso/www/training/pdf/race-ethnicity-onepager.pdf
- Hollander M, Wolfe DA. Nonparametric Statistical Methods. 2nd ed. Hoboken, NJ: Wiley; c1999.
- Brown AF, Liang LJ, Vassar SD, et al. Trends in racial/ethnic and nativity disparities in cardiovascular health among adults without prevalent cardiovascular disease in the United States, 1988 to 2014. Ann Intern Med 2018;168:541-9. [Crossref] [PubMed]
- Nahum-Shani I, Hekler EB, Spruijt-Metz D. Building health behavior models to guide the development of just-in-time adaptive interventions: A pragmatic framework. Health Psychol 2015;34S:1209-19. [Crossref] [PubMed]
- Schoeppe S, Alley S, Van Lippevelde W, et al. Efficacy of interventions that use apps to improve diet, physical activity and sedentary behaviour: A systematic review. Int J Behav Nutr Phys Act 2016;13:127-53. [Crossref] [PubMed]
- Maher CA, Lewis LK, Ferrar K, et al. Are health behavior change interventions that use online social networks effective? A systematic review. J Med Internet Res 2014;16:e40. [Crossref] [PubMed]
Cite this article as: Heron KE, Romano KA, Braitman AL. Mobile technology use and mHealth text message preferences: an examination of gender, racial, and ethnic differences among emerging adult college students. mHealth 2019;5:2.


