Interest in and barriers to participation in a Facebook-delivered weight loss program among female cancer survivors with overweight or obesity
Introduction
Improvements in cancer screening and treatment have contributed to a decline in cancer mortality rates for the majority of cancer types in the United States (1), resulting in a growing population of cancer survivors that is expected to reach more than 20 million by 2025 (2). This increase in survivorship has brought to light the need to address health-related concerns for survivors, including those associated with excess weight and insufficient physical activity: worsened prognosis, negative effects on quality of life, and increased mortality (3,4). Obesity has increased more rapidly among adult cancer survivors compared with the general population (5). Furthermore, the prevalence of class I obesity is consistently higher in female cancer survivors (14–21%) compared with women with no history of cancer (12–17%) (5). This is particularly meaningful for female cancer survivors because of the strong link between obesity and recurrence of breast, ovarian, and endometrial cancers (6-9).
Cancer survivors face many of the same barriers to healthy eating and exercise behaviors that individuals without a history of cancer do, such as family responsibilities, illness, work, transportation, the perception that exercise was too strenuous, no access to specific foods, and the cost of foods (10). Cancer survivors also face barriers specific to participating in exercise programs, including cancer-related fatigue, pain, neuropathy, treatment-related symptoms, and lack of information about how to safely perform exercise (11-13). Female cancer survivors put greater emphasis on additional barriers that male cancer survivors may not experience. Female survivors and women generally report that the traditional female caregiver role negatively impacts their ability to engage in physical activity (14,15). Addressing and overcoming barriers specific to female cancer survivors is important to increase the feasibility of success in a weight loss intervention.
Online interventions, such as those delivered via social media, offer a potentially appealing alternative to in-person interventions which can be challenging to participate in over a prolonged period of time. Facebook is the most popular social networking platform, and 79% of online US adults are active users (72% of adults ages 50–64 and 62% of adults aged 65 and older) (16). Recent research suggests cancer survivors are increasingly turning to online communities, such as Facebook and Twitter, to gain information and social support (17,18). In fact, nearly 90% of social media users aged 50 or older use Facebook and/or Twitter to find and share health information, and women are nearly three times more likely than men to seek health information on social media (18). Weight loss interventions using Facebook as a primary delivery modality for young adults have been found to be acceptable and feasible (19) but it remains unknown whether this type of program is appropriate for adult female cancer survivors, of whom 87% are at least 50 years old (2). However, acceptability and effectiveness of technology-based interventions for weight loss (20,21) and increasing physical activity (22) in older cancer survivors has been established. With increasing social media use for health among US adults, and its popularity among women in particular (23,24), it is important to understand how to leverage this technology to promote healthy lifestyle change among female cancer survivors.
Prior to the development of a weight loss program tailored for female cancer survivors, it is essential to explore the specific program needs and technology preferences of this population. We examined reasons women want to lose weight, barriers to and concerns about weight loss, preferences in weight loss intervention modality (i.e., in-person, telephone, Facebook, Twitter, private website) and specific components of a Facebook intervention, and preferences for group composition (cancer exclusive or not). The purpose of this study is to determine what female cancer survivors see as the most important components of a Facebook-delivered weight loss program to aid in the tailoring of such a program.
Methods
Study design
In 2016, we conducted a cross-sectional web-based survey of overweight or obese female cancer survivors who completed active treatment (e.g., chemotherapy, radiation, surgery). We recruited women using Twitter, Facebook, Craigslist, ResearchMatch, and internal online posts at our institution from February 2016 to June 2016. Recruitment ads, including Facebook posts, tweets using relevant hashtags, and general posts, targeted women with a history of cancer regardless of geographic location. Participants completed an online eligibility screener that asked about gender, age, if the individual ever had a cancer diagnosis, if the individual completed active cancer treatment (for example: chemotherapy, radiation, surgery), and if the individual was able to read, write, and speak English. After reading a fact sheet and providing consent, eligible individuals were directed to the survey (25). The survey contained items created in-house to examine specific interests of female cancer survivors based on interactions the authors had with this population. Participants who provided their emails at the end of the survey had a 2 in 100 chance of winning a $25 online gift card. The University of Massachusetts Medical School Institutional Review Board approved this study.
Measures
Reasons for wanting to lose weight
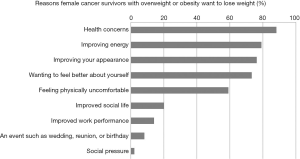
Participants were asked to select all of the reasons they wanted to lose weight from a predefined list (i.e., health concerns, improving your appearance, social pressure, wanting to feel better about yourself, an event such as a wedding, reunion or birthday, improved energy, improve social life, improved work performance, feeling physically uncomfortable).
Weight loss barriers and concerns
Participants were asked about perceived barriers to weight loss: “how much do you believe that trying to lose weight will result in too much sacrifice/burden (e.g., not enough time, denying yourself food)?” and “to what extent have other health issues (e.g., pain, depression, chronic condition) delayed you trying to lose weight?” Response options were: not at all, a little, somewhat, or very much. Participants were also asked, “how much has your cancer diagnosis affected your motivation to lose weight?” Response options were: greatly decreased my motivation, somewhat decreased my motivation, it has not affected my motivation, somewhat increased my motivation, and greatly increased my motivation. Lastly, barriers and concerns regarding weight loss were assessed with two open-ended questions: “What are the biggest barriers to losing weight for you?” and “As a cancer survivor, when it comes to losing weight, what is your biggest concern?”
Preferences in intervention modality and components
We then described a 3-month Facebook-delivered weight loss intervention designed for female cancer survivors: “We would like to know your opinions about a 3-month weight loss program that is conducted online. The program would be specifically designed for female cancer survivors. Over 3 months, you and the other cancer survivors in the program would receive dietary and exercise coaching to help you meet your weight loss goals in a secret Facebook group. This secret group is very private – only those who have been invited to the group can join, find the group, and see who else is a member of the group. We would ask you to set goals and report progress and challenges on a regular basis. You would be able to ask questions to the group and expert weight loss counselors.” Participants rated their interest in this program on a scale from 0 (not at all interested) to 10 (extremely interested). Participants also rated their interest in alternative program delivery methods (i.e., weekly in-person clinic visits, telephone calls, Twitter, a private website other than Facebook) on a scale from 0 (not at all interested) to 10 (extremely interested). Because the number of responses on some of the scales were low, we categorized the responses as 0 (not at all interested), 1–4 (a little bit interested), 5 (neither uninterested nor interested), 6–9 (quite a bit interested), and 10 (extremely interested). Next, we provided participants with a list of program components and asked to select all that were of interest to them (e.g., having it led by a weight loss counselor, being able to interact with a cancer survivor who successfully lost weight after her diagnosis, links to healthy recipes, getting support from other cancer survivors who are trying to lose weight). Lastly, participants were asked an open-ended question about interest in other features of a Facebook-delivered intervention: “What other features would you like in a weight loss program designed specifically for cancer survivors that is done in a private Facebook group?”
Participants self-reported demographics, cancer history, and social media, online weight loss program experience, and weight loss application (“app”) use.
Analysis
Using independent-samples t-tests and a one-way ANOVA, we examined differences in interest in a Facebook-delivered weight loss program by previous online weight loss program use, mobile weight loss app use, and frequency of Facebook use. We calculated body mass index (BMI) from self-reported height and weight, and categorized women by BMI class as recommended (26). We included only overweight or obese survivors in the analytic sample because we aim to design an intervention for women whose health would benefit from weight loss.
Sample characteristics, barriers to weight loss, and the proportion interested in the each of the delivery methods and specific program components were summarized. Thematic analyses were used to characterize responses to the open-ended questions (27). Two coders (CN May, M Evan) independently reviewed all responses to identify major themes. The coders discussed the themes and refined them. Responses were independently coded using these themes. Inter-rater reliability was good (28) (barriers: 93% agreement, k=0.90; concerns: 88% agreement, k=0.63; features: 96% agreement, k=0.84). Lastly, coders discussed discrepantly coded responses until they reached consensus. All analyses were conducted in 2016 using SPSS version 23 (29).
Results
Of the 208 participants who clicked on the survey link to get information about the study, 193 (93%) consented to participate, 7 (3%) declined to participate, and 8 (4%) exited the webpage without indicating informed consent. Most (78%) of those who opted to participate were eligible, 17% did not complete the eligibility questions, and 5% were ineligible [haven’t completed active treatment (n=8), never been diagnosed as having cancer (n=2), sex (n=1), and not fluent in English (n=1)]. Of the 162 eligible survivors, we excluded women who were normal weight (n=45), underweight (n=2), or missing height and/or weight information (n=19), resulting in an analytic sample of 96 overweight or obese female cancer survivors.
Participant characteristics
Participant characteristics are reported in Table 1. The sample (mean age = 54.3±9.6 years) was highly educated (72% completed at least a bachelor’s degree), and majority non-Hispanic (96%), and white (89%). Most participants (71%) were breast cancer survivors and 14% reported cancer at multiple sites. Most participants (58%) completed treatment one to ten years ago. Approximately 11% of survivors were still receiving maintenance therapy (i.e., treatment used to avoid or slow the return of cancer or to slow the growth of advanced cancer after initial treatment). Participants had a mean BMI of 32.7±5.8 kg/m2; 34% were overweight and 66% were obese. The majority (87%) had intentionally tried to lose weight in the past year. The majority of participants owned a smartphone (92%); 96% had Facebook account, and 88% reported checking it at least once per day. Fifty-one percent had a Twitter account and 17% checked it at least once per day. Thirty-one percent had ever tried an online weight loss program and 39% had used a mobile app to help them lose weight.

Full table
Reasons for wanting to lose weight
The reasons for women wanting to lose weight are presented in Figure 1. The majority (88%) of participants selected health concerns as a reason they wanted to lose weight. Most participants also selected wanting to improve energy (79%), improve appearance (76%), and feel better (73%; Figure 1). The least common reasons were: improved work performance (14%), an event such as a wedding, reunion, or birthday (8%), and social pressure (2%).
Weight loss barriers and concerns
Fifty-two percent of participants reported that other health issues (e.g., pain, depression, chronic condition) have delayed their weight loss efforts either “somewhat” or “very much”. Mental health was one of the major comorbidities for survivors and nearly one-quarter (24%) reported having depression or another psychiatric disorder. Slightly more than one-third of survivors (35%) reported that trying to lose weight will result in too much sacrifice/burden. Fifty-eight percent reported a somewhat or greatly increased motivation to lose weight because of their cancer diagnosis, while 22% reported a somewhat or greatly decreased motivation.
Of the 96 participants surveyed, 89 provided a response to the open-ended question, “what are the biggest barriers to losing weight for you?” A total of 130 responses were condensed into 14 codes (Table 2). The most common themes were making dietary changes/portion control (19%), lack of motivation/will-power (18%), physical limitations (13%), too tired/ low energy (12%) and perceived lack of time/too busy (11%). Seventy-one survivors provided responses to “as a cancer survivor, when it comes to losing weight, what is your biggest concern?” Eighty-one responses were condensed into 11 categories (Table 2). The most frequently reported concerns were fear of cancer recurrence (20%), previous weight loss failure/unsure of weight loss success (17%), and difficulty of weight loss due to treatment effects (12%).
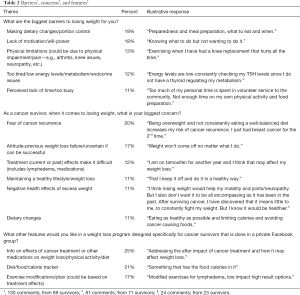
Full table
Preferences in intervention modality and components
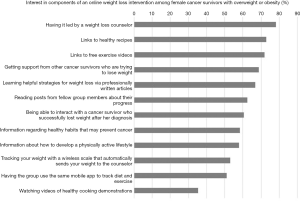
On a scale from 0 to 10, participants were most interested in participating in a weight loss program that was delivered via Facebook (mean =7.5±2.3) or via a private website other than Facebook (mean =6.6±3.3). Survivors were somewhat interested in weekly in-person meetings (mean =4.3±3.4) and telephone calls (mean =4.2±3.4). A Twitter-delivered program was of least interest (mean =2.4±3.1; Table 3). Most participants (78%) were quite a bit comfortable (49%) or extremely comfortable (29%) with using their personal Facebook accounts to participate in a weight loss intervention delivered via a secret Facebook group. Three-quarters (78%) were interested in a Facebook group led by a weight loss counselor; the majority of participants were also interested in access to links to healthy recipes (73%) and free exercise videos (72%; Figure 2). The program component garnering interest from the smallest proportion of participants was watching videos of healthy cooking demonstrations (35%; Figure 2). Twenty-three participants provided a response to “What other features would you like in a weight loss program designed specifically for cancer survivors that is done in a private Facebook group?” Twenty-four responses were condensed into 9 categories (Table 2). The most common responses included wanting information on effects of cancer treatment or other medications on weight loss (25%), access to a calorie tracker (21%), and specific exercise modifications/plans (17%).
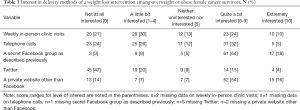
Full table
Individuals who had previously used an online program to help them lose weight were more interested in a Facebook-delivered weight loss program (mean =8.4±2.0) than individuals who had never tried an online weight loss program [mean =7.0±2.4; t(91)= −2.90, P=0.005]. There were no significant differences in interest level for a Facebook-delivered weight loss program among individuals who had previously used a mobile app who help them lose weight (mean =7.9±2.1) compared with those who had never used a mobile app [mean =7.2±2.2; t(91)= −1.58, P=0.119]. There were no significant differences among the different groups of Facebook use frequency on interest in the Facebook-delivered weight loss program [F(4,85)=1.05, P=0.388].
Overall, 43% of participants wanted to participate in a Facebook group that included survivors of any type of cancer, 19% preferred a group with survivors of the same type of cancer, 3% wanted a group that was not specifically focused on cancer survivors, and a 33% did not have a strong preference.
Discussion
Over three-quarters of overweight or obese female cancer survivors in our sample reported interest in a Facebook-delivered weight loss program tailored for female cancer survivors. Even though only about 40% of participants had ever tried an online program to help them lose weight, survivors were most interested in a Facebook-delivered weight loss program. Participants with previous experience using an online program for weight loss were more interested in a Facebook-delivered weight loss program than those with no experience. Therefore, individuals who have used online programs see their value and are interested in this delivery modality. Although previous users of online programs were more interested in a Facebook-delivered program, non-users were still quite interested in this type of program, suggesting that the benefits of a Facebook program may outweigh the hesitation to participate from a lack of mobile weight loss program experience.
Research has shown that adults are generally already using online social networks to share their weight loss experiences, provide social support, and to hold each other accountable (30). Among breast cancer survivors, one study surveyed participants in the #bcsm (breast cancer social media) patient community on Twitter and found that participants felt more informed and less anxious about their diagnosis as a result of participating in the community (17). Given that nearly 90% of online survivors are using social media to learn about survivorship and elicit support (18), it is not surprising that female cancer survivors preferred a Facebook-delivered weight loss program. Just under half of survivors (43%) in our sample preferred other Facebook group members to have a history of any type of cancer and 33% had no strong preference about the cancer history of group members, suggesting that a weight loss program could be designed for the needs and challenges of female cancer survivors generally but may not require tailoring for specific cancer types.
Given that lack of time and being too busy were commonly reported barriers to losing weight, Facebook may be effective to circumvent the burden of attending in-person visits. Older adults are increasingly joining Facebook with 62% of adults 65 years or older being current users, which is a 14-point increase from 48% in 2015 (16). On average, Facebook users spend an average of 50 minutes per day on it (31), making it an ideal method for delivering intervention content within participants’ daily routines. Participating in a Facebook intervention, compared to a traditional in-person intervention, is less disruptive to daily/weekly routines and would provide survivors with in-the-moment opportunities to engage with other participants and weight loss experts.
In addition to lack of time, female cancer survivors also face unique challenges to weight loss that need to be addressed in weight loss programs. Over half of survivors in this study reported that other health issues (e.g., pain, depression, chronic condition) delayed weight loss attempts, and qualitative data revealed that physical limitations, such as arthritis and neuropathy, posed significant barriers to losing weight. This is consistent with previous research that health-related issues, such as neuropathy, pain, and fatigue are barriers to weight loss among adult cancer survivors (13). Women who participated in the survey also wanted more information about how cancer treatments and medications could affect their weight loss. Therefore, future online programs should include this kind of information for survivors. Among middle-aged women without a history of cancer, lack of time and caregiving duties are cited as two of the top perceived barriers to physical activity (32). Therefore, physical limitations appear to be larger barriers to physical activity for cancer survivors compared to middle-aged women generally. Because these physical limitations likely impede physical activity (10), and in turn weight loss, it is not surprising that some survivors reported wanting specific information on how to modify exercise to accommodate their limitations. In the rheumatoid arthritis literature, symptoms of the disease such as pain and fatigue, are seen as barriers to physical activity but physical activity is viewed as a means to reduce pain and fatigue (33). Therefore, individualized tailoring of the physical activity portion of a weight loss program for cancer survivors may be necessary to insure that all participants know how to safely perform these activities. By providing cancer survivors with information about how physical activity can help reduce their pain and fatigue and specific instructions for making adjustments to accommodate their physical limitations may reduce barriers to physical activity and increase overall health.
Limitations of this study include the convenience sample - the majority of which was non-Hispanic white and highly educated, which limits generalizability. Online recruitment likely resulted in a sample of survivors who are more interested in participating in an online weight loss program compared to survivors who did not participate, and a sample more likely to represent technology literate survivors compared to survivors generally. The target population for an online social media intervention would include individuals who are established users of these platforms, so these results likely represent the perspectives of the target population. Also, internet and social media use continue to grow rapidly in older adults and female cancer survivors (17,18) and the appeal of online interventions may also grow. Additionally, it is possible that participants responded to the survey multiple times because we did not collect respondents’ IP addresses (34). However, this is unlikely because the incentive for participants to complete more than one survey was small. We also relied on self-reported height and weight to calculate BMI. Self-reported weight tends to be an underestimate of actual weight (35), but research has shown that web-based self-reports of weights and heights are valid (36).
In summary, over three-fourths of survivors were interested in and preferred a Facebook-delivered weight loss intervention tailored to address the needs of survivors compared to other delivery methods. Health issues, including physical limitations, were the largest barriers for survivors to attempt weight loss. This study addresses an important gap in the female cancer survivor literature by acknowledging preferences and barriers to creating a tailored online weight loss program for this population. Online weight loss programs have the potential to reach a larger number of cancer survivors because of the lack of geographic and scheduling constraints of traditional in-person interventions. Future research should focus on developing an effective weight loss program delivered via Facebook to overcome weight loss barriers specific to female survivors, including physical limitations and continued health concerns.
Acknowledgments
Funding: This work was supported by National Institutes of Health grants R25CA172009 and 1T32HL120823-01.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: All procedures were approved by the University of Massachusetts Medical School Institutional Review Board. The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
References
- Lerro CC, Stein KD, Smith T, et al. A systematic review of large-scale surveys of cancer survivors conducted in North America, 2000-2011. Journal of Cancer Survivorship 2012;6:115-45. [Crossref] [PubMed]
- Miller KD, Siegel RL, Lin CC, et al. Cancer treatment and survivorship statistics, 2016. CA Cancer J Clin 2016;66:271-89. [Crossref] [PubMed]
- Calle EE, Rodriguez C, Walker-Thurmond K, et al. Overweight, Obesity, and Mortality from Cancer in a Prospectively Studied Cohort of U.S. Adults. N Engl J Med 2003;348:1625-38. [Crossref] [PubMed]
- Eheman C, Henley SJ, Ballard-Barbash R, et al. Annual Report to the Nation on the status of cancer, 1975-2008, featuring cancers associated with excess weight and lack of sufficient physical activity. Cancer 2012;118:2338-66. [Crossref] [PubMed]
- Greenlee H, Shi Z, Sardo Molmenti CL, et al. Trends in obesity prevalence in adults with a history of cancer: Results from the US National Health Interview Survey, 1997 to 2014. J Clin Oncol 2016;34:3133-40. [Crossref] [PubMed]
- Arem H, Irwin ML. Obesity and endometrial cancer survival: a systematic review. Int J Obes (Lond) 2013;37:634-9. [Crossref] [PubMed]
- Demark-Wahnefried W, Peterson B, McBride C, et al. Current health behaviors and readiness to pursue life-style changes among men and women diagnosed with early stage prostate and breast carcinomas. Cancer 2000;88:674-84. [Crossref] [PubMed]
- Demark-Wahnefried W, Platz EA, Ligibel JA, et al. The role of obesity in cancer survival and recurrence. Cancer Epidemiol Biomarkers Prev 2012;21:1244-59. [Crossref] [PubMed]
- Nagle CM, Dixon SC, Jensen A, et al. Obesity and survival among women with ovarian cancer: Results from the Ovarian Cancer Association Consortium. Br J Cancer 2015;113:817-26. [Crossref] [PubMed]
- Aycinena AC, Valdovinos C, Crew KD, et al. Barriers to Recruitment and Adherence in a Randomized Controlled Diet and Exercise Weight Loss Intervention Among Minority Breast Cancer Survivors. J Immigr Minor Health 2017;19:120-9. [Crossref] [PubMed]
- Puszkiewicz P, Roberts AL, Smith L, et al. Assessment of Cancer Survivors’ Experiences of Using a Publicly Available Physical Activity Mobile Application. JMIR Cancer 2016;2:e7. [Crossref] [PubMed]
- Blaney J, Lowe-Strong A, Rankin J, et al. The Cancer Rehabilitation Journey: Barriers to and Facilitators of Exercise Among Patients With Cancer-Related Fatigue. Phys Ther 2010;90:1135-47. [Crossref] [PubMed]
- Beehler GP, Rodrigues AE, Kay MA, et al. Perceptions of Barriers and Facilitators to Health Behavior Change Among Veteran Cancer Survivors. Mil Med 2014;179:998-1005. [Crossref] [PubMed]
- Hefferon K, Murphy H, McLeod J, et al. Understanding barriers to exercise implementation 5-year post-breast cancer diagnosis: A large-scale qualitative study. Health Educ Res 2013;28:843-56. [Crossref] [PubMed]
- World Health Organization (WHO). Physical Activity and Women 2010. Available online: http://www.who.int/dietphysicalactivity/factsheet_adults/en/
- Greenwood S, Perrin A, Duggan M. Social Media Update 2016. Pew Research Center 2016. Available online: http://assets.pewresearch.org/wp-content/uploads/sites/14/2016/11/10132827/PI_2016.11.11_Social-Media-Update_FINAL.pdf
- Attai DJ, Cowher MS, Al-Hamadani M, et al. Twitter Social Media is an Effective Tool for Breast Cancer Patient Education and Support: Patient-Reported Outcomes by Survey. J Med Internet Res 2015;17:e188. [Crossref] [PubMed]
- Tennant B, Stellefson M, Dodd V, et al. eHealth literacy and Web 2.0 health information seeking behaviors among baby boomers and older adults. J Med Internet Res 2015;17:e70. [Crossref] [PubMed]
- Waring ME, Jake-Schoffman DE, Holovatska MM, et al. Social Media and Obesity in Adults: a Review of Recent Research and Future Directions. Curr Diab Rep 2018;18:34. [Crossref] [PubMed]
- Haggerty AF, Huepenbecker S, Sarwer DB, et al. The use of novel technology-based weight loss interventions for obese women with endometrial hyperplasia and cancer. Gynecol Oncol 2016;140:239-44. [Crossref] [PubMed]
- Cadmus-Bertram L, Nelson SH, Hartman S, et al. Randomized trial of a phone- and web-based weight loss program for women at elevated breast cancer risk: the HELP study. J Behav Med 2016;39:551-9. [Crossref] [PubMed]
- Hong YA, Goldberg D, Ory MG, et al. Efficacy of a Mobile-Enabled Web App (iCanFit) in Promoting Physical Activity Among Older Cancer Survivors: A Pilot Study. JMIR Cancer 2015;1:e7. [Crossref] [PubMed]
- Duggan M, Brenner J. The Demographics of Social Media Users-2012. Washington, DC Pew Res Center’s Internet Am Life Proj 2013;2013:1-14.
- We are Flint. Percentage of female internet users in the United States who access selected social networks as of January 2018. Statista - The Statistics Portal. Available online: https://www.statista.com/statistics/249802/percentage-of-female-us-internet-users-who-use-social-networks/
- Harris PA, Taylor R, Thielke R, et al. Research electronic data capture (REDCap)—A metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 2009;42:377-81. [Crossref] [PubMed]
- NHLBI Obesity Education Initiative Expert Panel on the Identification, Evaluation, and Treatment of Obesity in Adults (US). Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report. Bethesda (MD): National Heart, Lung, and Blood Institute; Available online: https://www.ncbi.nlm.nih.gov/books/NBK2003/
- Pope C, Mays N. Reaching the parts other methods cannot reach: an introduction to qualitative methods in health and health services research. BMJ 1995;311:42-5. [Crossref] [PubMed]
- Landis JR, Koch GG. The Measurement of Observer Agreement for Categorical Data Data for Categorical of Observer Agreement The Measurement. Biometrics 1977;33:159-74. [Crossref] [PubMed]
- IBM Corp. Released 2015. IBM SPSS Statistics for Windows, Version 23.0. Armonk, NY: IBM Corp.
- Pagoto S. The current state of lifestyle intervention implementation research: Where do we go next? Transl Behav Med 2011;1:401-5. [Crossref] [PubMed]
- D’Onfro, Jillian. Here’s how much time people spend on Facebook, Instagram, and Messenger every day. Business Insider 2016. Available online: https://www.businessinsider.com/how-much-time-do-people-spend-on-facebook-per-day-2016-4
- King AC, Castro C, Wilcox S, et al. Personal and environmental factors associated with physical inactivity among different racial-ethnic groups of U.S. middle-aged and older-aged women. Health Psychol 2000;19:354-64. [Crossref] [PubMed]
- Veldhuijzen van Zanten JJCS, Rouse PC, Hale ED, et al. Perceived Barriers, Facilitators and Benefits for Regular Physical Activity and Exercise in Patients with Rheumatoid Arthritis: A Review of the Literature. Sports Med 2015;45:1401-12. [Crossref] [PubMed]
- Quach S, Pereira JA, Russell ML, et al. The good, bad, and ugly of online recruitment of parents for health-related focus groups: Lessons learned. J Med Internet Res 2013;15:e250. [Crossref] [PubMed]
- Stommel M, Schoenborn CA. Accuracy and usefulness of BMI measures based on self-reported weight and height: Findings from the NHANES & NHIS 2001-2006. BMC Public Health 2009;9:421. [Crossref] [PubMed]
- Bonn SE, Lagerros YT, Bälter K. How valid are web-based self-reports of weight? J Med Internet Res 2013;15:e52. [Crossref] [PubMed]
Cite this article as: May CN, Jake-Schoffman DE, Evans M, Silfee VJ, Zhang FF, Blok AC, Carey JL, Ding E, Pritschmann RK. Interest in and barriers to participation in a Facebook-delivered weight loss program among female cancer survivors with overweight or obesity. mHealth 2019;5:28.